Retrospective analysis suggests MendelScan saves 3.5 years of medical and financial burden in Behçets disease
Diagnostic Dilemma
Behçet's disease is a rare chronic multisystem disorder characterised by recurrent ulcers, painful joints and life threatening complications involving the central nervous system and major blood vessels. Confirming a diagnosis is difficult as there is no specific test and the disease symptoms overlap with several disorders like Inflammatory Bowel Disease. During their diagnostic odyssey, most patients endure numerous investigations and specialist referrals to rule out other illnesses while undergoing symptomatic treatment. Repeated clinical visits and hospitalizations often lead to loss of wages and rise in unemployment among patients. Behçet's patients also have difficulty with everyday functioning with a 45% reduction in their health related quality of life compared to the general UK adult population. Early diagnosis can significantly impact three areas namely the length of time in getting the right diagnosis, improvement in quality of life and the financial cost to the family and the health system.
Advances in early diagnosis
Mendelian is focussed on shortening the diagnostic odyssey of rare diseases by using patients’ Electronic Health Records (EHRs). The software tool, MendelScan, highlights potential rare disease patients using our own algorithm and outlines the next steps that can be taken to confirm the diagnosis based on established clinical care guidelines. By empowering GPs to address the complexity of rare disease diagnosis, Mendelian ultimately improves patient care while reducing resource utilisation.
Economic impact
Rare diseases are a significant economic burden in the UK, with 10% of the total NHS budget in 2016 spent on specialised services for rare diseases. In 2018, in collaboration with Imperial College Health Partners, Mendelian commissioned a study to understand the economic impact of rare disease diagnostic delay. This demonstrated that the cost of rare disease patients hospital activity is an average of £13,000 per patient over a 10 year period, double the cost of an average patient. Previous research suggests the annual direct cost per patient with Behçet's is $2,203 with diagnostic tests and medications contributing to 96% of the direct medical costs. As primary care costs are expected to be a substantial component of the costs incurred in the Behçet's disease diagnostic process, we performed the following analysis to explore the healthcare utilisation in the primary care setting, with a focus on the three years before the diagnosis.
Methodology
The Electronic Health Records of Behçet's disease patients were evaluated and analysed retrospectively to determine the primary care costs and diagnostic odyssey years potentially saved by Mendelian’s approach in diagnosing Behçet's disease patients. Healthcare resource utilisation was measured based on CTV3 codes. Direct medical costs included were based on published literature and national tariffs.
Saving years and costs
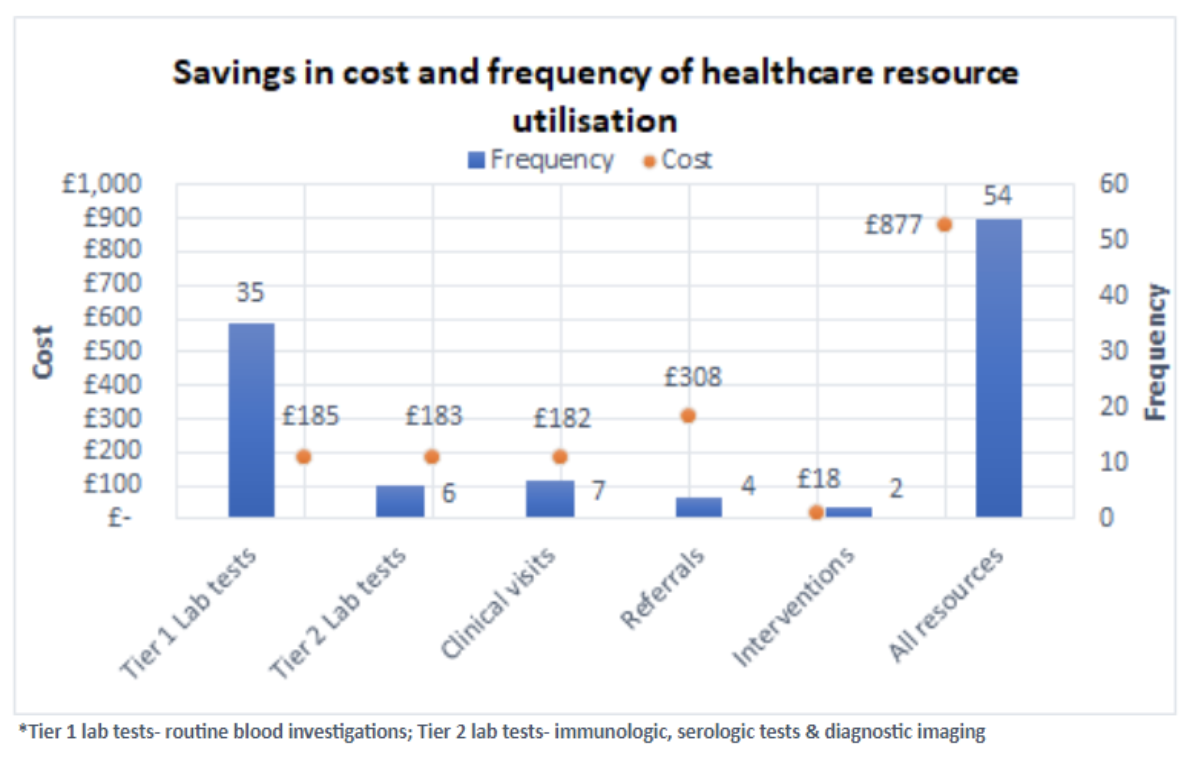
Our results demonstrate that MendelScan can save on average 3.5 years of a patient’s diagnostic odyssey, resulting in a significant saving of £876 incurred in the three years before diagnosis. As a result , on average 41 laboratory tests, 7 clinical visits and 4 specialist referrals during this 3 year period. With the additional benefits of reducing the workload for primary care providers and time and emotional distress for the patients, these findings demonstrate that MendelScan can potentially save both time and costs in the diagnostic odyssey of Behçet's disease.
Getting ahead
MendelScan enables clinicians to diagnose rare diseases faster by highlighting patients with possible rare diseases based on established diagnostic criteria. Our retrospective EHR analysis for Behcet’s disease, has demonstrated that Mendelian’s MendelScan can shorten the diagnostic odyssey by 3.5 years, reduce primary healthcare utilisation costs by £876, and significantly improve the rare disease diagnostic journey. Our results add further strength to the fact that timely diagnosis has a significant positive economic impact in primary care and potentially secondary care.
If you liked this article maybe you will also find interesting the following in-depth articles about other rare diseases, like A Day In The Life Of...Holly Ward A Day In The Life Of...Hadley Mahon Speaker Series - Leber Congenital Amaurosis